Aging in Community
Programs 284, 285, 286, 287
CDs available via special order. HumanMedia ®
Also available on our Podcast
Programs 284, 285, 286, 287
CDs available via special order. HumanMedia ®
Also available on our Podcast
Within a decade, America will be looking different. In addition to other demographic changes, 70 million Baby Boomers are now entering their retirement years. For the first time in our history, there will be more older adults than children.
This huge societal change will affect how families provide eldercare, how older Americans access transportation, and whether people can age in their own homes among neighbors they know — and avoid nursing facilities, where about 30% of Covid-19 deaths occurred.
These shifts will accelerate a trend that began three decades ago with passage of the Americans with Disabilities Act: local communities are attempting to become more age-friendly. What changes will this mean for how families relate, how our streets and sidewalks are designed, how we use technology?
On Aging in Community, a special project from Humankind public radio, you’ll hear stories of transition and dignity — and meet people who are showing the way.
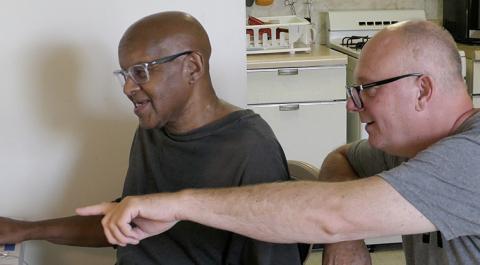
Melvin Lewis (L) with Dave Sevick, Computer Reach
I think the biggest problem is isolation. [Older adults] don’t feel connected to the community or their families.”
— Dave Sevick
Supported by The RRF Foundation for Aging, The John A. Hartford Foundation and The Boston Foundation, and by the Humankind Program Fund. In association with Documentary Educational Resources and WGBH/Boston. Recording engineer: Antonio Oliart Ros. Communication Director: Jacques Klapisch. Special thanks to Connie Goldman, Ken Rogers, Noel Flatt, David Cruz, Brian K. Johnson, Cathy Graham, Steve Martin, Jake Cavicchi, Laura Carlo, Haggerty Media, Wesley Family Services and Tony Buck.

Laura Poskin, Age-Friendly Greater Pittsburgh
The American Association of Retired Persons (AARP) has cited the region around Pittsburgh, Pennsylvania as especially attentive to the needs of older adults.
Through a series of events called the Crossings, sponsored by Age-Friendly Greater Pittsburgh, local activists have worked with city officials to make crossing the street safer for elders. It was a relief for one older woman who for years had been afraid to venture into the crosswalk at her building, since several neighbors had been hit by cars there.

Patricia Hill (L) and Ally Evelyn-Gustave, CAPABLE
Another need being addressed by a local Pittsburgh-area nonprofit, Computer Reach, is online access, which became practically a lifeline for older adults when the coronavirus struck. We also meet a volunteer who regularly visits a retired man, helping him shop, do errands and provide friendly company, through Wesley Family Services.

Jim Schultz (L) and volunteer Mark Hall
And we visit the home of a Baltimore-area elder, who benefitted from an innovative free service known as CAPABLE, operated by Johns Hopkins University, which provides an occupational therapist, a nurse and a handyworker to modify the homes of older residents to improve safety.
Aging in your community is possible for a lot of people, but you have to have the supports, the infrastructure to be able to do that.”
— Laura Poskin
From the moment we [occupational therapists] step on a person’s front porch, we are looking for things that could cause a problem, whether it’s a shaky rail or a slippery step.”
— Ally Evelyn-Gustave

Jill Hall, Baltimore County Dept. of Aging
We’ll meet members of the Seven Oaks Senior Center outside Baltimore. Nearly 10,000 of these centers now operate across the United States, serving over a million older adults each day. They have become a vibrant fixture of age-friendly communities. Many offer classes, social events, exercise equipment, and a network of friends — who become important, especially if a member has lost a spouse or re-located from elsewhere.

Jon Duvall, Veterans Administration and Univ. of Pittsburgh
The vast majority of older adults experience one or more health challenge. We’ll hear the story of Jon Duvall, PhD, a researcher in assistive technology, who is a wheelchair user. He draws on his experience surviving a spinal cord injury. At the Univ. of Pittsburgh Human Engineering Laboratories, Jon develops and tests devices that help people with disabilities, including elders, to participate in society.

Janet Seckel-Cerrotti, FriendshipWorks
We also learn about the history of federal programs, including Social Security and Medicare, that have been established to help Americans sixty-five or older and remain remarkably popular with the public.

Edwin Walker, Deputy Asst. Secy. for Aging, HHS
And we chat with a woman who has devoted her life to serving older adults, including her efforts at FriendshipWorks, a Boston-based program, which matches elders with usually younger companions. She aims to foster greater connections, which can counteract loneliness often experienced by older adults living alone.
[At senior centers] you can volunteer, you can teach, you can just socialize with people.”
— Jill Hall
It was actually my doctor who said, ‘Have you considered rehab engineering?’”
— Jon Duvall


Jacqueline Boyd,
The Care Plan (Chicago)
Millions of adult children or other relatives are caring for older loved ones. They do this out of love, but the cumulative burden can be heavy. It often adds up to a lot of time, it can take a toll on the caregiver’s finances, and it almost always brings worry. More than one in five American adults is in the role of a caregiver for an elder — usually a parent or grandparent or spouse.
Mary Jo Kreitzer,
Prof. of nursing, Univ. of MN,
Bakken Ctr. for Spirituality & Healing
Some older folks receive help with typical needs of aging: doctors appointments, grocery shopping, managing medications, paying bills. Over 3 million (a number expected to rise) are living with some form of dementia.

Bonnie Pelletier, attends caregiver support group
(Plainville, CT)
There are joys in taking care of someone who’s important to you, but there can also be times of intense strain. We’ll hear stories of how different families manage the duties of eldercare. We also include useful suggestions from a leading professor of nursing on how caregivers can benefit from proven techniques of self-care.
“If I get a call during the day, my heart drops. I just think, ‘What happened?’”
—Ronda Guberman
Everything is on my plate, everything, 24 hours a day.”
—Bonnie Pelletier
I have been going to all of my mother’s doctors appointments. My calendar’s like just crazy.”
—Steve Brennan
Caregivers are dealing with feelings of guilt that they’re not doing enough.”
—Jacqueline Boyd
Wherever we go, [Mom is] always included, so she’s kept very busy, which keeps her going.”
—Mary Corbett

Anthony Hopkins in The Father
Nearly 5 million direct care workers assist America’s older adults. They perform their duties in private homes, residential care settings and nursing facilities. An example of this was movingly dramatized in The Father, Anthony Hopkins’ Academy Award-winning role as an older man under care, who was overcome by bewilderment.
This workforce is projected to expand dramatically as the population of elders surges. Nine in ten are women, mostly people of color and immigrants.

Martina Cummings (L) and Jesse Dunbar,
Direct care workers (Chicago area) Mary Mathis, photo
And, says PHI, which tracks these employees: “they are consistently marginalized”. Often paid low wages, many rely on some form of public assistance to make ends meet. A surprising number are homeless. Yet the labor can be arduous, helping sometimes disabled people with dressing, toilet care, mobility challenges, transferring in and out of bed. And sometimes the clients they serve are angry, even abusive.

David Grabowski,
Prof. of health care policy, Harvard
We’ll listen to the stories of some of these workers. And you’ll meet several experts in this field, including the director of the WaCares Fund, a first in the nation program in Washington State, attempting to make eldercare more affordable for families.
This has been the greatest education: understanding people and understanding how we are all connected.”
—Martina Cummings, Eldercare worker
You’re spending a full day with someone who may have cognitive impairment.”
—David Grabowski, Harvard Medical School
Over the long term, you need a structural solution so that there’s a system in place.”
—Ben Veghte, WaCares Fund (Washington State)